Author: Catherine Loveday, University of Westminster
American actor Bruce Willis has frontotemporal dementia, his family has announced.
In 2022, the 67-year-old action movie star was diagnosed with aphasia – difficulty with language and speech. Aphasia can occur for a variety of reasons (most commonly stroke) but for Willis, it is now clear that these speech problems were the early signs of this particularly devastating form of dementia.
Frontotemporal dementia is an umbrella term for any disease that causes gradual loss of brain tissue in the frontal and temporal lobes – the front and sides of the brain. Although relatively rare, it is one of the most common causes of dementia in people under the age of 65, accounting for around 40% of early-onset cases.
The condition – which goes by other names, such as Pick’s disease, frontal dementia, semantic dementia and primary progressive aphasia – tends to develop slowly, over several years.
A build-up of abnormal proteins affects critical brain areas, leading to changes in behaviour, personality and speech. Unlike other forms of dementia, such as Alzheimer’s disease, memory is often only affected later in the disease’s progression.
There are three different variants of frontotemporal dementia: the “behavioural variant”, “non-fluent variant primary aphasia” and “semantic variant primary aphasia”. Each of these will initially present differently and can be mistaken for other conditions.
The earliest signs of the behavioural variant include changes in how a person acts, particularly in social situations. They may become tactless or make rash decisions. Or they may behave inappropriately, for example, by making sexual advances. Some may develop obsessive ritualistic behaviour, or lose all sense of empathy and caring.
These symptoms reflect damage to the frontal lobes, an area of the brain involved in directing our behaviour, controlling our impulses, managing our emotions and generating speech and movement.
When they stop working, people tend to lack insight into their own behaviour or how they have changed. Their relatives find it particularly hard because they can’t have frank conversations with their loved ones as they can’t see what the problem is.
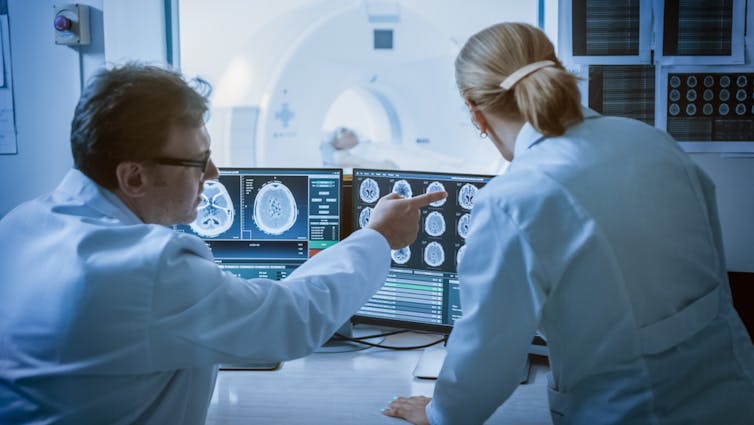
Diagnosis can be difficult because these symptoms also occur in other conditions where the frontal lobes are injured, such as strokes and tumours, so a full medical history and brain scans play an important role. To make things even more tricky for doctors, there is also significant overlap with several psychiatric disorders – for example, depression, schizophrenia and obsessive-compulsive disorder. This can lead to misdiagnosis or a missed diagnosis, especially in the early stages of the disease.
We don’t know which variant Willis has been diagnosed with, but his family has reported that his earlier symptoms relate to difficulties with speech, a feature that is typically seen at the onset of the other two variants. In these cases, there is a gradual loss in the ability to speak and understand language.
As the disease progresses, brain cells across the frontal and temporal lobes are destroyed. And, regardless of the variant, people will eventually experience many of the symptoms above. This is accompanied by increasing difficulty with walking and moving. By the end, most struggle to eat and swallow.
Frontotemporal dementia is a devastating and life-changing disease for which we have no cure and little in the way of treatment. For now, the focus is on managing symptoms and maximising quality of life. This may involve helping people develop ways to manage their emotions and behaviour, or drugs such as antidepressants and antipsychotics.
Genes provide clues
There is some room for hope. In recent years, scientists have made progress in understanding more about which brain cells are being affected. One in eight sufferers will have frontotemporal dementia in the family, and important clues about the disease process are emerging from detailed analysis of the genetics.
The key now is to translate this research into earlier and better diagnosis, and ultimately to develop drugs that will halt or reverse this devastating disease.
Catherine Loveday, Professor, Neuropsychology, University of Westminster
This article is republished from The Conversation under a Creative Commons license. Read the original article.
- Obesity as a genotoxic environment - April 28, 2023
- Dalit History Month and its significance - April 20, 2023
- A professor is going to live in an underwater hotel for 100 days – here’s what it might do to his body - April 13, 2023
